Cervical cancer: symptoms, causes and early detection
Cervical cancer at a glance
The term cervical cancer understandably raises concerns. However, this type of cancer does have positive aspects: Its cause is known, you can protect yourself against it and, thanks to regular cervical cancer screening at your gynaecologist’s practice, the chances of detecting cervical cancer early and treating it promptly are good.
What exactly is cervical cancer?
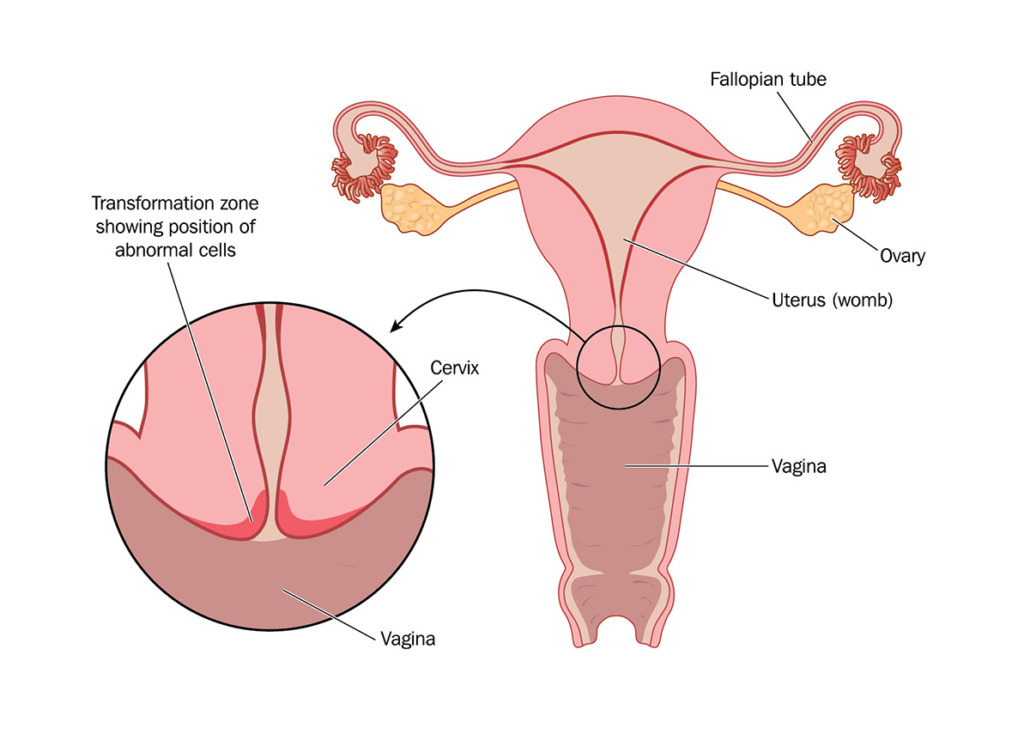
Tumors that develop on the cervix are called cervical cancer or cervical carcinoma. The cervix, technically known as the uterine cervix, is the lower part of the uterus. It is the connection between the uterus and the vagina.
Cervical cancer develops via precursors. Initially, cell changes only occur on the surface of the cervix. Once deeper cells are affected, then cancer could be present.
Does HPV cause cervical carcinoma?
In almost all cases, human papillomaviruses, or HPV for short, are responsible for the development of cervical carcinoma.
Nevertheless, an HPV infection is no reason to panic! Almost every woman is infected with the virus at least once in her life. This is because of its sexual transmission and the fact that condoms do not offer sufficient protection.
In 90 out of 100 cases, the body’s own immune system can fight an HPV infection and no damage remains.
Cervical cancer usually only develops if the infection lasts for years and if the infection involves so-called high-risk HPV types. In this case, cell changes can occur in the mucous membrane of the cervix.
A slight cell change is not necessarily a bad thing, as the affected areas can also regenerate completely. However, if the cell changes worsen and become precancerous, a cervical carcinoma can develop. This process takes between seven to ten years. So if you go for regular screenings, there is a good chance of detecting cervical cancer at an early stage.
Preventing cervical cancer – the HPV vaccination
The special thing about cervical cancer is that its cause is known and there is a way to protect yourself with the HPV vaccination, which is effective against certain high-risk HPV types.
Ideally, the HPV vaccination should be carried out before the first sexual intercourse. The Standing Committee on Vaccination recommends vaccinating girls and boys between the ages of nine and fourteen.
Although the HPV vaccination is often mentioned in connection with cervical cancer, it also makes sense for boys! Not only does it protect their sexual partners later on, but HPV can also trigger other types of cancer and diseases.
But be careful: the vaccination protects against certain high-risk HPV types, but not against all. For this reason, regular cervical cancer screening is also important for vaccinated women!
Early detection: HPV test and Pap smear
Early detection is very successful, because cervical cancer develops slowly. Ideally, treatment of precancerous lesions can begin and the altered cells will be caught before they can develop into cervical cancer.
In Germany, there is an organized cervical cancer screening program. This consists of two stages:
- Women between the ages of 20 and 34 are entitled to a Pap smear or Pap test once a year.
- Women aged 35 and over can go for co-testing every three years. This is a combination of a Pap smear and an HPV test.
The costs of the Pap smear and HPV test are covered by health insurance as part of the early detection of cervical cancer.
HPV test
For the HPV test, the gynecologist swabs a sample from the cervical mucosa. Women do not normally notice the difference between the Pap and HPV tests. A laboratory then determines whether human papillomaviruses are present.
Pap test
For the Pap test, a gynecologist takes a smear from the mucous membrane of the cervix. To do this, they insert an instrument that looks like a long cotton bud or brush. The sample is then sent to a laboratory and examined under a microscope for cell changes.
What symptoms does cervical cancer cause?
Cell changes or precancerous lesions in the cervix do not usually cause any symptoms. For this reason, it makes sense to go for regular screenings as it’s the only way to detect and treat the silent danger at an early stage.
The following symptoms may indicate cervical cancer:
In most cases, affected women only notice symptoms once the precancerous lesions have developed into cervical cancer. Tumors on the cervix can cause the following symptoms:
- Intermenstrual bleeding, often after sexual contact
- Unusually heavy menstruation
- Foul-smelling discharge
- Pain in the pelvic area
Abnormality in cervical cancer screening: what happens next?
Normally the rule is: no news is good news. In most cases, the doctor’s office only contacts you if abnormalities were found during cervical cancer screening.
Abnormalities can be
- The HPV test is positive
- The Pap smear is abnormal
HPV-positive or abnormal Pap test
The affected woman should first try to remain calm: an HPV infection or an abnormal Pap test is not a cancer diagnosis! They merely indicate an increased risk of cancer. Further steps are necessary for a confirmed diagnosis:
- Wait and schedule another appointment: Depending on the degree of abnormality, it may be sufficient to repeat the examination after a certain period of time.
- colposcopy (cervical endoscopy): During a colposcopy, the cervix is examined using a special microscope. Changes in the tissue can be visualized and, if necessary, a tissue sample can be taken (biopsy). Not every gynecologist’s office offers this examination. Affected women often have to make an appointment with a specialist at a so-called dysplasia consultation.
- Conization: During conization, the abnormal pieces of tissue are removed from the cervix in a cone shape and then examined pathologically. This method is therefore used for both diagnosis and treatment. If the affected area is small, it can be completely removed by conization.
- Test based on epigenetic biomarkers: GynTect is suitable for clarifying abnormalities in cervical cancer screening. It is a test that not only looks at the cell, but also examines the DNA of the cell. To do this, the gynecologist takes a swab from the cervix and sends it to a laboratory.
Der GynTect® Test
Quick verification
in case of suspected
cervical cancer
Conclusion
Cervical cancer, a tumor formation on the lower part of the uterus, is caused by a long-lasting infection with human papillomavirus (HPV). But there is good news! If you pay attention to two important points, you can protect yourself against cervical cancer:
First, early detection pays off! It takes years for an HPV infection to develop into cervical cancer. By going for regular check-ups, you have a good chance of detecting cervical cancer in its preliminary stages and successfully treating it.
Secondly, the HPV vaccination protects against cervical cancer! The vaccination is particularly effective if it is given before the first sexual contact. However, it is important to note that the vaccination does not replace a screening examination.
Order GynTect®
Contact us, to get GynTect®
On request, you will receive a free smear test kit, which is accompanied by a treatment contract. Only when we the lab received the swab sample together with the signed examination request in the laboratory do you undertake to pay the costs of the test.
Do you have any further questions? Please use the contact options provided.
Epitype GmbH
Löbstedter Str. 41
07749 Jena
Germany
Contact us if you have any further questions:
Picture credits
- Title: Fotogrin / Shutterstock.com
- Female genitalia graphic: Lamb / Shutterstock.com
- Graphic of woman with female genitals: Zubada / Shutterstock.com